Introduction: When Every Step Hurts
Think about how awful it would be to get up every day and dread the moment your feet hit the floor. Millions of individuals throughout the world deal with stabbing, scorching agony in their heels every day. A heel spur is typically to blame. Knowing the appropriate heel spurs therapy can make the difference between persistent pain and lasting relief, whether you’ve just been diagnosed or have been dealing with this condition for years.
This complete guide tells you all you need to know about heel spurs, including what they are, why they happen, and, most importantly, the best treatments that are backed by research. By the conclusion, you’ll have a clear, doable plan for getting back to moving without pain.
What Are Heel Spurs? A Clear Definition
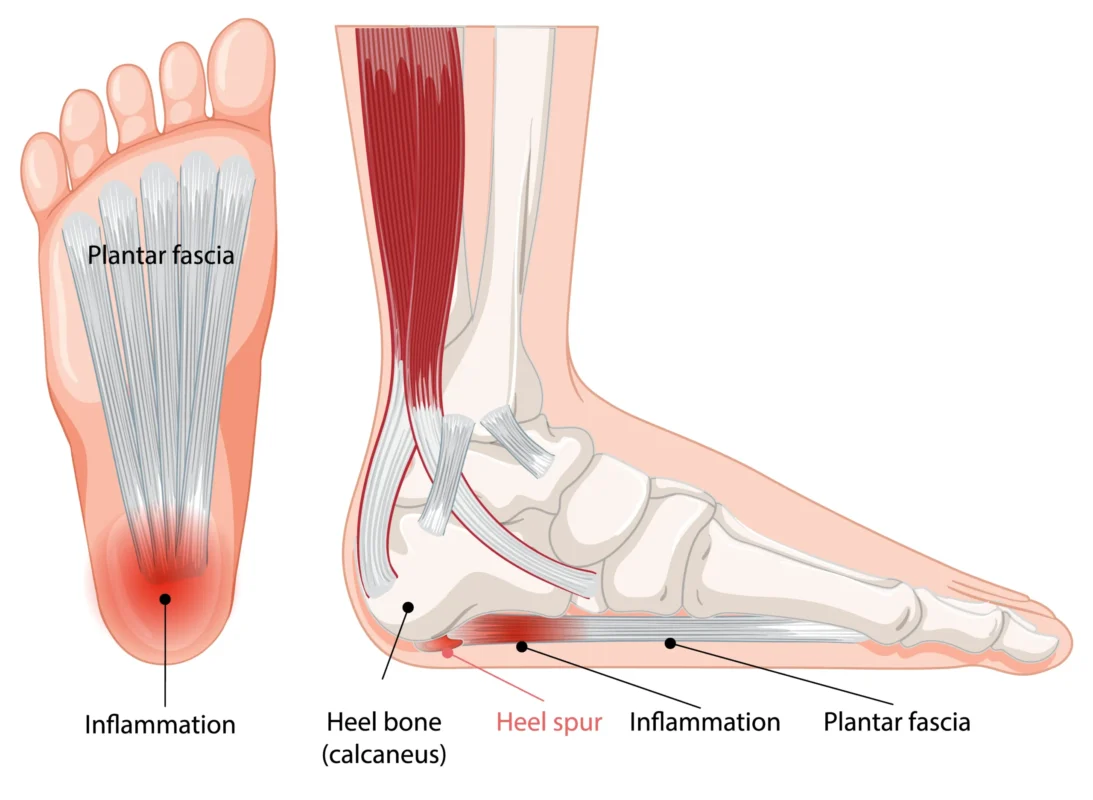
A heel spur (also referred to as a calcaneal spur) is a bony calcium deposit located on the underside of your heel bone (calcaneus). Over time, it develops slowly due to high amounts of stress on its muscles and ligaments in the foot.
- Important Fact: The American Academy of Orthopaedic Surgeons (AAOS) says that roughly 10% of people have heel spurs, although only about 5% of those people feel pain from the spur itself.
It’s easy to mix up heel spurs and plantar fasciitis, and that’s for a good reason. There is a strong connection between the two circumstances. The pain is mostly caused by plantar fasciitis, which is inflammation of the band of tissue that runs down the bottom of the foot. The spur is usually a subsequent development. As a group, they are one of the most prevalent reasons adults have heel discomfort.
Who Is Most at Risk? Understanding the Causes
Before starting treatment for heel spurs, it’s helpful to know what causes them in the first place. There are a number of risk factors that play a role:
- Too much exercise, such as running, jogging, or standing for lengthy periods of time
- Obesity or an abrupt weight increase might put more pressure on the heel.
- Worn-out shoes or shoes that don’t support the arch well
- Flat feet or high arches can cause the plantar fascia to be strained because of how you walk.
- Age: Most people who have it are between 40 and 60 years old.
- Diabetes—linked to a greater frequency of foot issues
- Occupational hazards—Teachers, nurses, retail workers, and sports workers are particularly susceptible.
Diagnosing Heel Spurs: What to Expect
An accurate diagnosis is key when treating heel spurs. A podiatrist or orthopaedic expert typically will:
- Check your medical history and how active you are
- Do a physical assessment by pressing on certain parts of the heel to find pain.
- Get an X-ray. This is the only sure method to find out if there is a bone spur and how big it is.
Use an ultrasound or MRI (if necessary) to check for soft tissue injury and rule out other disorders. Dr. Amelia Torres, DPM, a board-certified podiatrist and foot health specialist, says, “Just because you have a heel spur on an X-ray doesn’t mean it’s the source of your pain.”
Heel Spurs Therapy: A Step-by-Step Treatment Roadmap
A tiered strategy is used in effective heel spur therapy. This means starting with less invasive, more conservative procedures and only moving on to more aggressive ones when needed. This is the full breakdown:
First-Line Heel Spurs Therapy — Conservative Treatments
According to the AAOS, more than 90% of heel spur cases become better with conservative treatment within 10 to 12 months. These are your top and first choices.
1. Rest and Activity Modification
Taking some weight off the heel provides the irritated tissue time to heal. This doesn’t imply lying in bed all day; it involves managing your activities wisely:
- Change from high-impact sports like running and jumping to low-impact ones like swimming and biking.
- Don’t walk barefoot on hard surfaces.
- During long shifts, take pauses to sit down often.
2. Ice Therapy
Putting ice on the heel helps with swelling and numbs the pain.
How to do it:
- Put a small cloth around an ice pack or a bag of frozen peas.
- Put it on your heel for 15 to 20 minutes, three to four times a day.
- Never put ice directly on your skin; it might cause frostbite.
3. Stretching Exercises
One of the best ways to treat heel spurs is with targeted stretching. It eases tightness in the Achilles tendon and plantar fascia.
Most effective stretches include:
- To stretch your plantar fascia, sit down, cross one leg over the other, and gently draw your toes back toward your shin. Keep it for 30 seconds. Do it three times for each foot.
- Calf stretch (standing wall stretch): Put your hands on a wall and one foot in front of the other. Keep your back knee straight and your heel on the floor. Gently lean forward. Hold for 30 seconds.
- Before getting out of bed, wrap a towel over your foot and draw your toes toward you for 30 seconds. This is part of your morning routine.
Pro tip: Do these stretches before you get out of bed in the morning. This is when the discomfort is usually at its worst.
4. Orthotic Insoles and Supportive Footwear
Custom or over-the-counter orthotic insoles help the plantar fascia and move pressure away from the heel spur. A study published in the Journal of Foot and Ankle Surgery indicated that 72% of individuals who used orthotic devices had less heel discomfort within three months.
What to look for in footwear:
- Deep heel cups for comfort
- Strong support for the arch
- A small rise in the heel (1–1.5 cm)
- Stay away from flat-soled shoes, flip-flops and going barefoot on hard floors.
5. Anti-Inflammatory Medications (NSAIDs)
Ibuprofen and naproxen are examples of nonsteroidal anti-inflammatory drugs (NSAIDs) that can aid with pain and swelling for a short time. But these just help with the symptoms, not the cause, and using them for a long period can hurt your stomach.
Before starting any drug, you should always talk to your doctor.
Intermediate Heel Spurs Therapy Options
When first-line treatments don’t work, the next step is to try intermediate therapies that are stronger and more focused.
6. Physical Therapy
When first-line treatments don’t work, the next step is to try intermediate therapies that are stronger and more focused.
- Manual therapy is when you use your hands to move joints and soft tissue.
- Ultrasound therapy uses sound waves to help heal deep tissue.
- Taping methods, such as kinesiology taping, take tension off the plantar fascia.
- Gait analysis and retraining fix the biomechanical problems that led to the spur.
7. Night Splints
Night splints keep your foot in a slightly dorsiflexed (toes-up) position as you sleep. This slowly stretches the plantar fascia. Studies show that night splints can significantly improve the morning symptoms of people with plantar fasciitis and heel spurs.
- Worn for one to three months
- Can be bought pre-made or made to match your needs
- At first, you may feel a little uncomfortable, but the pain shouldn’t be too bad.
8. Corticosteroid Injections
For chronic, moderate-to-severe pain, corticosteroid (cortisone) injections straight into the heel can provide swift relief by diminishing inflammation.
| Feature | Corticosteroid Injection |
| Onset of relief | 24–72 hours |
| Duration of effect | 4–12 weeks |
| Maximum recommended | 2–3 injections per year |
| Risks | Plantar fascia rupture, fat pad atrophy (with repeated use) |
These are not a cure; they only provide you a “window” of relief so that rehabilitation can go more smoothly.
Advanced Heel Spurs Therapy for Resistant Cases
Fewer than 10% of patients need more complex treatments. These choices might be right for you if you’ve been using conservative therapy for 6 to 12 months and it hasn’t helped enough.
Extracorporeal Shock Wave Therapy (ESWT)
ESWT is one of the best non-surgical treatments for heel spurs that we know of. It uses high-energy sound waves to help damaged tissue repair and break away calcium deposits.
Clinical evidence is strong:
- A meta-analysis published in PLOS ONE in 2020 showed that 60–80% of people with recurrent plantar fasciitis or heel spurs were successful.
- FDA-approved for plantar fasciitis that doesn’t go away
- Not invasive and done in an outpatient setting
- Needs 3 to 5 sessions over the course of 3 to 5 weeks
Possible adverse effects include temporary bruising, swelling, and minor pain during treatment.
10. Platelet-Rich Plasma (PRP) Therapy
PRP therapy entails taking a small sample of the patient’s blood, concentrating the healing platelets, and injecting them into the tissue around the heel that is hurt. It speeds up the body’s natural healing process.
- Recent research indicates similar or enhanced outcomes compared to corticosteroid injections, with fewer long-term hazards.
- Needs one to three shots
- More expensive; insurance doesn’t always cover it.
11. Surgical Intervention (Last Resort)
Only after 12 months of trying all alternative treatments for heel spurs and failing can doctors consider surgery. There are two main steps:
- Plantar fascia release: Partially cutting the plantar fascia to reduce tension (most common)
- Surgery to remove a heel spur (spur resection): This involves taking off the bony spur.
Important: Surgery usually works well, but it can cause nerve damage, a longer recovery time (3–6 months), and a chance of coming back.
Comparison Table: Heel Spurs Therapy Options at a Glance
| Therapy | Invasiveness | Cost | Time to Relief | Best For |
| Rest & Ice | None | Free | Days to weeks | Acute, mild pain |
| Stretching | None | Free | Weeks | All stages |
| Orthotics | None | Low–Moderate | Weeks | Biomechanical issues |
| Physical Therapy | Minimal | Moderate | 4–8 weeks | Moderate cases |
| Night Splints | None | Low | 4–12 weeks | Morning pain |
| NSAIDs | Oral | Low | Days | Short-term relief |
| Corticosteroid Injection | Minimally invasive | Moderate | 24–72 hours | Severe acute pain |
| ESWT | Non-invasive | Moderate–High | 4–12 weeks | Chronic, resistant cases |
| PRP Therapy | Minimally invasive | High | 4–8 weeks | Chronic cases |
| Surgery | Invasive | High | 3–6 months | Refractory cases only |
Lifestyle Changes That Supercharge Heel Spurs Therapy
Making changes to your lifestyle at the same time as getting treatment for heel spurs makes the treatment much more effective. These things aren’t frills; they are necessary for long-term rehabilitation.
- Managing your weight: Every extra kilogram puts about 3–4 times more stress on your heels when you walk. Even losing a little weight can make a big difference in how much tension is on your heels.
- Shoe rotation: Change the pressure locations on your feet by wearing different pairs of supportive shoes.
- Always do a 5-minute warm-up before working out. Cold, stiff muscles and fascia are much more likely to get hurt.
- Toe curls, marble pickups, and single-leg calf raises are all foot-strengthening exercises that work the intrinsic muscles that support the arch.
- Change out your old sneakers often. Running shoes should be replaced every 500 to 700 kilometers.
Key Takeaways
- The best time to start heel spur therapy is as soon as possible. Don’t wait until the pain gets worse.
- Stretching, orthotics, and rest are all conservative treatments that work for more than 90% of instances.
- Stretching is the one habit you can practice every day that will make the biggest difference.
- Surgery is only needed in rare cases and should only be done after 12 months of unsuccessful treatment.
- For long-term success, you must adjust your lifestyle (weight, shoes, and activities).
- Before starting any kind of therapy, you should always receive a good diagnosis.
FAQ: Heel Spurs Therapy — Your Questions Answered
Q1: How long does it take for heel spur treatment to work?
Most people start to feel better after 4 to 8 weeks of persistent conservative treatment. Usually, it takes 6 to 12 months for full resolution. ESWT and other advanced therapies may work in 4 to 6 weeks.
Q2: Do heel spurs go away on their own?
Without therapy, the bony spur itself doesn’t often go away. But with the right treatment for heel spurs, the discomfort can go away completely. Most individuals don’t need to have the spur removed to feel better.
Q3: Is it good or bad to walk with heel spurs?
Walking lightly in shoes that give you support is usually good for you. Walking on hard surfaces with a lot of impact without the right cushioning makes inflammation worse. Instead of halting all activities, listen to your body and change what you’re doing.
Q4: Do home remedies work for heel spur pain?
Yes, stretching, ice, over-the-counter orthotics, and rest are the main parts of early heel spur treatment and work very well for mild to moderate instances.
Q5: What is the greatest shoe to wear if you have heel spurs?
Choose shoes with a deep heel cushion, strong arch support, and a small heel lift. Podiatrists often recommend the following brands: HOKA, Brooks, New Balance (1540 series), and Vionic.
Q6: Can I work out with heel spurs?
Yes, but with changes. Swimming, biking, yoga, and working out your upper body are all great choices. Don’t sprint, jump, or stand on hard floors for long periods of time until your symptoms are better.
Q7: Will my heel spur come back after I have treatment?
It can, especially if the root causes (bad shoes, biomechanical problems, too much weight) aren’t fixed. To keep the problem from coming back, you need to keep stretching and wear the right shoes.
Conclusion: Your Path to Heel Pain Relief Starts Now
You don’t have to become used to living with heel spur discomfort. The good news is that heel spur therapy works very well, and most individuals get better without having to have surgery. The most important thing is to have a planned and consistent plan. Start with conservative treatments, stick to daily stretching, get good shoes, and, if necessary, increase treatment under the advice of a professional.
Don’t let the pain get worse before you do something about it. Make an appointment with a podiatrist or orthopedic doctor immediately. Then, tomorrow morning, start your stretching routine. This is the first step toward a life without pain.
Your heels carry you through life, so it’s time to take care of them.
Sources and Further Reading
Clinical & Academic References
American Academy of Orthopaedic Surgeons (AAOS) — Plantar Fasciitis and Bone Spurs
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) — Heel Pain
- Trojian, T., Tucker, A.K. (2019) — Plantar Fasciitis. American Family Physician.
- Goff, J.D., Crawford, R. (2011) — Diagnosis and Treatment of Plantar Fasciitis. American Family Physician.
- Landorf, K.B. et al. (2006) — Effectiveness of Foot Orthoses to Treat Plantar Fasciitis: A Randomized Trial. Archives of Internal Medicine.
Reputable Health Resources
- Mayo Clinic — Heel Pain Overview
- Cleveland Clinic — Heel Spurs
- NHS UK — Heel Pain (Plantar Fasciitis)
- WebMD — Heel Spurs Guide
Podiatry Today — Clinical Practice Resources

Nicola Donelan, PhD, brings more than 20 years of deep scientific expertise and over a decade of dedicated medical writing to every project she touches. Her work sits at the intersection of rigorous research and clear, purposeful communication — turning complex bioscience, pharmaceutical, and healthcare knowledge into content that informs, persuades, and performs.
From peer-reviewed journal articles and regulatory submissions to white papers, investor presentations, and healthcare communications, Nicola delivers writing that meets the highest standards of accuracy without sacrificing readability. She works with independent physicians, biotech innovators, pharmaceutical firms, and academic institutions — adapting her voice and approach to suit each client’s unique needs and audience.