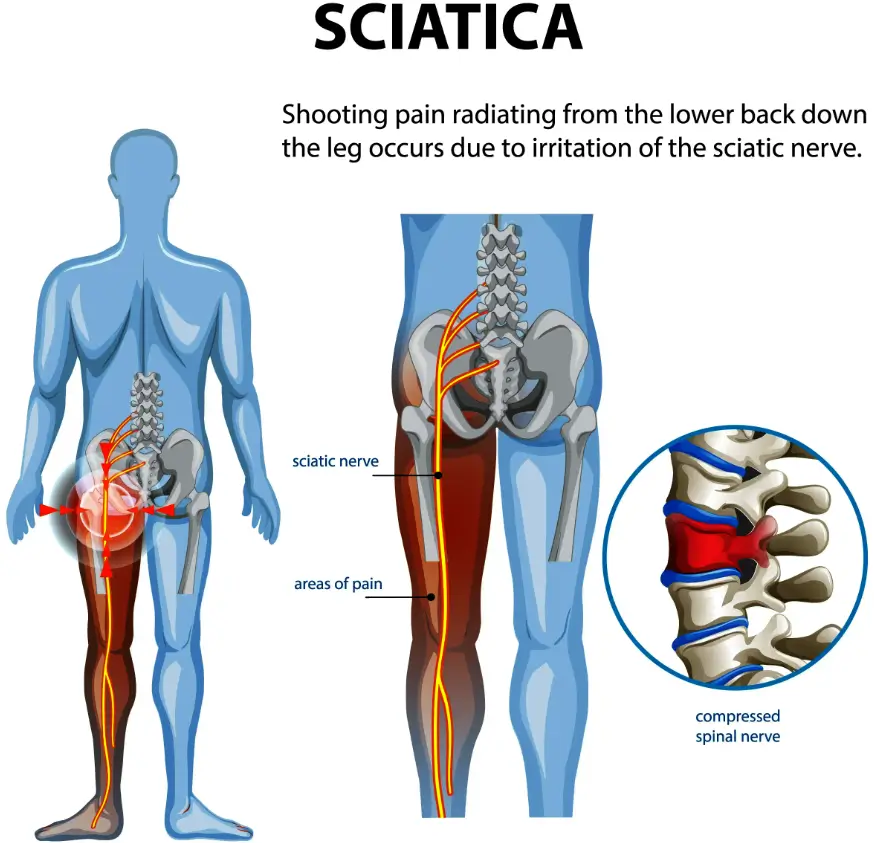
Why Physical Therapy Is the Gold Standard for Sciatica Relief
If you’ve ever had a searing, burning pain shoot down your leg from your lower back, you know how bad sciatica can be. The good news is? Physical therapy is still one of the best ways to get long-term relief from sciatica without having to have surgery or take medication for a long time.
This detailed guide will show you exactly how physical therapy treats the underlying reasons of sciatica, which techniques work best, and how to create a personalized program that gets you back to your normal routine as soon as possible. This article can help you get better, no matter when your symptoms started, whether it was last week or months ago.
- 40% of people will get sciatica at some point in their lives.
- 90% of sciatica cases get better with conservative care.
- 6–12 weeks is the typical time it takes to recover with structured physical therapy.
What Is Sciatica? Understanding the Condition Before Treatment
Sciatica is not an illness in its own right; rather it refers to a series of symptoms caused when one or more nerves travel down each leg from your lower spine down towards each foot and become pinched or irritated – be that from herniated discs, bone spurs or even Piriformis syndrome pinching it and leading to radiating pain which characterises sciatica as its signature feature.
Knowing what caused your sciatica is very important since it will help you choose the best sort of physical therapy for sciatica. Before making your program, a good physical therapist will always look at the main reason.
Common Causes of Sciatica
- Herniated or bulging lumbar disc: the most common cause, responsible for up to 90% of instances
- Lumbar spinal stenosis occurs when the spinal canal gets narrower, which puts pressure on nerve roots.
- Piriformis syndrome: The piriformis muscle in the buttocks puts pressure on or irritates the sciatic nerve.
- Spondylolisthesis: One vertebra slides forward on top of another, making the nerve outlet smaller.
- Degenerative disc disease – discs that break down with age, making them less comfortable
- Sacroiliac joint dysfunction—swelling at the pelvic joint that feels like sciatica
How Treatment for Sciatica Physical Therapy Works: The Core Principles
The basic idea behind physical therapy for sciatica is to find the mechanical problem that is putting pressure on or irritating the nerves and then fix it using targeted movement, manual techniques, and education. Painkillers merely cover up the symptoms, while physical therapy for sciatica works on the structural and muscle imbalances that are causing your discomfort.
Most physical therapy programs typically consist of three parts: managing acute pain, active rehabilitation and maintenance/prevention. Each step builds upon itself to restore strength, flexibility and function slowly but steadily.
Physical therapy serves to do more than alleviate pain; its goal is also to restore neuromuscular control and structural integrity to help avoid future episodes of sciatica.
Phase 1: Acute Pain Management Techniques
When sciatica pain is at its worst, the first thing to do is to calm down the nerves and reduce the swelling so that active rehabilitation can start. During this phase, your physical therapist will use a variety of passive and semi-active methods.
Manual Therapy and Hands-On Techniques
Manual therapy includes a variety of hands-on treatments that a professional physical therapist can perform.Research disseminated in the Journal of Orthopaedic & Sports Physical Therapy are available here. have repeatedly confirmed its effectiveness as an approach for treating sciatica within physical therapy.
- Spinal mobilization: mild, back-and-forth movements of the lumbar vertebrae to make the joints less rigid and more flexible.
- Soft tissue massage—focused manipulation on the piriformis, gluteal, and paraspinal muscles to relieve tension and ease nerve impingement
- Neural mobilization (nerve flossing) – gentle sliding and tensioning procedures that help break up adhesions on the sciatic nerve
- Myofascial release is when you put pressure on fascial limitations for a long time to make the tissue move again.
Modalities for Pain and Inflammation Control
- Transcutaneous electrical nerve stimulation (TENS) is a low-level electrical current that stops pain signals.
- Ultrasound therapy—strong thermal and mechanical effects that help tissues repair
- Ice and heat therapy: Ice for short-term inflammation (48–72 hours) and heat to relieve muscle spasms after that.
- Traction therapy is the mechanical or manual decompression of lumbar discs to reduce nerve pressure.
“Passive modalities are a bridge, not a destination. Our goal is always to get patients moving again as soon as their pain allows.” — Dr. Sarah Michaels, DPT, a doctor who specializes in orthopedics.

Phase 2: Active Rehabilitation — The Core of Sciatica Physical Therapy
This stage is the most important part of sciatica physical therapy. Once your acute pain goes down enough, your therapist will help you with a planned program of therapeutic exercises that will decompress the sciatic nerve, strengthen the muscles that support it, and get your typical movement patterns back.
McKenzie Method: Extension-Based Exercise
The McKenzie Method, or Mechanical Diagnosis and Therapy (MDT), is one of the most well-researched ways to treat sciatica with physical therapy. It entails recognizing directional movements that centralize (bring pain closer to the spine) and alleviate leg discomfort.
- Prone press-ups: Lying face down and pushing the upper body up while keeping the pelvis level. This helps the lumbar spine extend, and the discs move into a better position.
- Standing back extensions—done while standing up, these are very helpful for people who sit for lengthy periods of time.
- The whole program is based on the exact direction that works best to lessen symptoms. This is the direction that people should move in over and over again.
Core Stabilisation Exercises
A weak or poorly coordinated core puts too much stress on the lumbar spine and intervertebral discs. So, building deep core stability is a must for effective treatment for sciatica physical therapy.
- Dead bug: a supine exercise that trains deep abdominal co-activation while moving the limbs
- Bird dog: a four-legged exercise that helps keep the spine stable by extending the opposite limb.
- The Pallof press is an anti-rotation core exercise that strengthens the transverse abdominis.
- Abdominal bracing drills—teaching how to control pressure inside the abdomen correctly
Hip and Gluteal Strengthening
Patients with sciatica often have weak hip abductors and external rotators, and physical therapy for sciatica should include working on this. Strong gluteal muscles help the lumbar spine by lowering shear forces and taking pressure off the piriformis.
- Clamshells work the gluteus medius and the external hip rotators.
- Side-lying hip abduction—gradually making the lateral hip stabilizers stronger.
- Single-leg glute bridges work the hip extensors and the pelvic stability at the same time.
- Resistance band lateral walks are a way to develop the hip abductor muscles.
Nerve Mobilisation (Sciatic Nerve Flossing)
Neural mobilization techniques are one of the most unique parts of physical therapy for sciatica. These moderate workouts move the sciatic nerve through the tissues around it, which helps reduce adhesions and make the nerve more flexible without making the symptoms worse.
- Seated sciatic nerve floss: Sit up straight, straighten one knee while looking up, then bend the knee and gaze down. Do this in a rhythmic, pain-free way.
- Supine nerve slider: While resting on your back, bend your knee and hip to 90 degrees, then slowly extend your knee while bending your foot back.
- Standing nerve tensioner: for patients who have moved on from the acute phase; done with more nerve loading
Comparing Physical Therapy Approaches for Sciatica
Not all physical therapy methods work the same for everyone. The table below shows the most frequent methods side by side so you may talk to your therapist about which ones are best for you.
| Technique | Best For | Evidence Level | Typical Duration |
| McKenzie Method | Discogenic sciatica; centralisation of symptoms | High (RCTs) | 6–8 weeks |
| Neural Mobilisation | Nerve adhesions; chronic neurogenic pain | Moderate | 4–8 weeks |
| Core Stabilisation | Recurrent sciatica; spinal instability | High | 8–12 weeks |
| Manual Therapy | Acute pain; joint restrictions | Moderate–High | 3–6 weeks |
| Traction Therapy | Disc herniation with radiculopathy | Moderate | 4–6 weeks |
| Pilates-Based PT | Chronic sciatica; postural correction | Moderate | 8–16 weeks |
Phase 3: Maintenance, Prevention, and Long-Term Management
The last step in treating sciatica with physical therapy is to build on what you’ve learned and make yourself strong enough to avoid repeat occurrences. Studies suggest that patients who stick with a structured maintenance program have a lot lower rates of their symptoms coming back than those who cease therapy after their symptoms go away.
Postural Education and Ergonomic Correction
- Checking the workstation to make sure that the monitor, chair, and keyboard are all at the right height to reduce stress on the lower back
- Retraining your sitting posture—learning how to keep your lumbar lordosis when sitting for long periods of time.
- Lifting mechanics—learning the hip-hinge method to preserve the lower back while doing everyday chores
- Optimizing sleep position—advice on pillows and mattresses to reduce nerve compression while you sleep.
Home Exercise Programme
As part of your continuous treatment for sciatica, your physical therapist will provide you with a personalized home exercise program to follow. Being consistent with this regimen is the most crucial thing you can do to make sure you succeed in the long run.
- Do the exercises that have been given at least five days a week
- Gradually increase the intensity and difficulty of your workouts based on how your symptoms respond.
- Write down your symptoms in a journal to find out what activities or positions make them worse.
- During the maintenance phase, make an appointment with your therapist every four to six weeks.
Real-World Case Study: From Chronic Sciatica to Full Recovery:
The patient is a 42-year-old man who works in an office. Diagnosis: Herniated L4/L5 disc with sciatica on the right side. Symptoms lasted for 8 weeks before PT. Duration of treatment: 10 weeks of twice-weekly sessions and a home program. Result: The VAS pain score went down from 8 out of 10 to 1 out of 10. Went back to work full-time in Week 6. Running started up again in Week 10—no recurrence at the 12-month follow-up. McKenzie extension protocol, neural flossing, gradual core stabilization, and fixing an ergonomic workplace are some of the main methods used.
When to Seek Treatment for Sciatica Physical Therapy
Most healthcare guidelines say that people with non-emergency sciatica should consult a physical therapist within the first 4 to 6 weeks of the problem starting. Early intervention is linked to greater results and a lower chance of long-term problems.
Signs That You Should See a Physical Therapist Promptly
- Pain that radiates below the knee, into the foot, or causes numbness and tingling
- Symptoms that last longer than four weeks without getting better
- Pain that makes it hard for you to move, stand, or do everyday things
- Having sciatica more than once a year
Red Flags Requiring Immediate Medical Attention
If you have any of the following, get emergency care right away:
Loss of control over the bladder or bowel, sciatica pain, weakness that gets worse in both legs, saddle anesthesia (numbness in the inner thighs and groin), or sciatica after an injury. These signs could mean that you have cauda equina syndrome, which is a medical emergency.
Frequently Asked Questions
How long does it take for physical therapy to help with sciatica?
Most people see a big difference in their sciatica after 4 to 6 weeks of regular physical therapy. Most people fully recover in 6 to 12 weeks, although this depends on how bad the symptoms are, what caused them, and how well you follow your home regimen.
Is physical therapy a better option than surgery for sciatica?
For most cases of sciatica, conservative treatment, such as physical therapy, works just as well as surgery after one to two years, and it has a lot fewer dangers and problems. Surgery is usually only suggested when conservative treatment hasn’t worked after 6 to 12 weeks or when neurological impairments are getting worse.
Is it possible to undertake physical therapy for sciatica at home?
It is usually best to start with a supervised in-clinic program because doing exercises wrong can make nerve complaints worse. Once your physical therapist has looked at your condition and taught you the right ways to do things, a structured home program is an important and useful aspect of treatment for sciatica physical therapy.
How many times do I need to go to physical therapy?
Most programs for treating sciatica last 6 to 10 weeks and have 12 to 20 sessions. Most of the time, there are 2 to 3 sessions per week. Your therapist will change how often you see them based on how well you are doing and how you respond to treatment.
What should I stay away from during physical therapy for sciatica?
- Exercises that make leg pain worse or feel the same as it does now (beyond mild, acceptable discomfort)
- Sitting still for a long time without taking breaks to move (every 20–30 minutes)
- Doing high-impact exercises like running until your therapist says it’s okay
- Deep forward bending with a loaded spine during the acute phase
- Not paying attention to neurological signs that are getting worse, including more weakness or numbness
Does insurance pay for physical therapy for sciatica?
Most countries and most health insurance companies will pay for physical therapy for sciatica if a doctor or orthopaedic expert says you need it. The number of sessions that are covered depends on the plan. Before starting therapy, always check your coverage.
Action Items for Your Sciatica Recovery
Your List of Things to Do to Get Better from Sciatica
- Get a correct diagnosis. Before starting any workout program, consult a certified physical therapist to find out what is causing your sciatica.
- Start early: the biggest results come from doing physical therapy for sciatica within the first 4 to 6 weeks.
- Stick to it: go to all of your scheduled sessions and do your home program every day.
- Use more than one method. The best programs combine manual treatment, therapeutic exercise, and teaching.
- Talk about your lifestyle—how you move, how much you move, and how much you do all affect how quickly you heal.
- Plan for maintenance—don’t stop therapy as soon as the pain goes away; finish the whole program to keep it from happening again.
Conclusion:
You don’t have to let sciatica control your life. Most people who get the appropriate kind of physical therapy for sciatica, from a professional therapist and with their entire commitment to the process, will fully and permanently recover. The most important thing is to make a plan that includes targeted manual treatment, gradual therapeutic exercise, and smart changes to your lifestyle that are right for your body and your goals.
Don’t wait for your sciatica to go away on its own. The longer nerve compression goes on without therapy, the more likely it is that you will have persistent pain and nerve damage that lasts. Call a professional physical therapist now, tell them exactly what your symptoms are, and take the first and most crucial step toward getting back to a pain-free, active life.
Sources and Further Reading
The following peer-reviewed studies, clinical guidelines, and authoritative resources informed the evidence base of this article:
- Suri, P., et al. (2011). Incidence of Symptomatic Lumbar Disc Herniation. Spine.
- Wirth, B., et al. (2021). Neurodynamic Techniques for Sciatica Journal of Manual & Manipulative Therapy.
- Garcia, A.N., et al. (2013). McKenzie Method Versus Manual Therapy for Lumbar Radiculopathy. Physical Therapy.
- American Physical Therapy Association (APTA). Clinical Practice Guideline: Low Back Pain. JOSPT, 2021.
- European Spine Journal. European Guidelines for the Management of Acute Nonspecific Low Back Pain.
- American Academy of Orthopaedic Surgeons (AAOS): Sciatica patient education resources
- PubMed (National Library of Medicine) — Search primary research on sciatica physical therapy

A retired physician with dual specialization in neurology and neurorehabilitation, Dr. Senelick spent 30 years as Medical Director of one of Texas’s leading rehabilitation hospitals — building clinical programs that have helped thousands of patients reclaim their lives after devastating neurological events.